Cerebal Palsy
Self-Help Information

What is Cerebal Palsy?
Cerebral palsy (CP) is a group of permanent movement and posture disorders caused by abnormal development or damage to the brain before, during, or shortly after birth.
- Prevalence: About 1 in 300 children worldwide are diagnosed with CP.
- Causes: Common contributors include premature birth, lack of oxygen (asphyxia), infections during pregnancy, and brain injuries in early infancy.
- Types: CP is classified by the primary motor pattern affected:
- Spastic CP – stiff, jerky movements (most common).
- Dyskinetic CP – involuntary, writhing motions.
- Ataxic CP – poor balance and coordination.
Impact: While the brain injury itself does not worsen over time, secondary issues such as muscle contractures, joint problems, and pain can develop if not managed early.
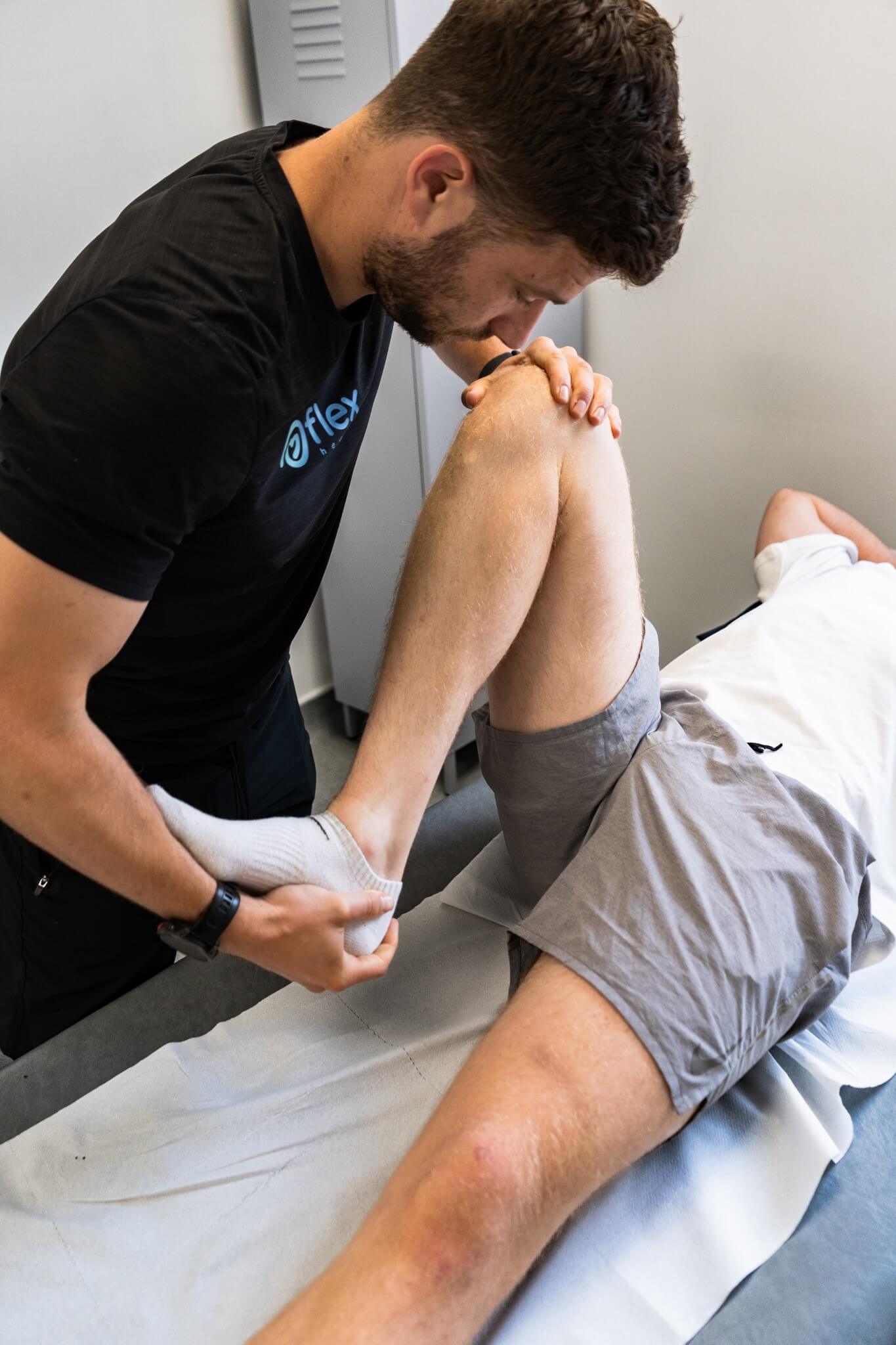
Cerebral palsy is a lifelong condition, but with appropriate therapy and support, most individuals lead active, fulfilling lives.
Core Treatment Options
Physical Therapy
Regular stretching, strengthening, and functional mobility exercises.
Medication
Muscle relaxants (e.g., baclofen, diazepam) or antispasmodics to reduce spasticity; anticonvulsants for seizure control.
Botulinum Toxin Injections
Temporary reduction of focal muscle tightness, often combined with therapy.
Assistive Devices
Braces, walkers, wheelchairs, or customized seating systems to improve independence.
Surgical Interventions
Tendon releases, selective dorsal rhizotomy, or orthopedic corrections for severe deformities.
Therapeutic Recreation & Sports
Adaptive swimming, horseback riding (hip‑polo), and inclusive athletics promote fitness and confidence.
Everyday Tips for Families & Caregivers
Maintain a consistent routine
Predictability helps manage fatigue and anxiety.
Encourage active play
Even short, frequent activity bursts support muscle health.
Monitor skin integrity
People who use wheelchairs are prone to pressure sores; reposition every 2 hours.
Stay hydrated & balanced nutrition
Adequate calories and fluids aid growth and muscle function.
Use technology
Speech‑generating devices, eye‑tracking software, and mobile apps can boost communication and learning.
Connect with support groups
Peer networks provide practical advice and emotional encouragement.
Customer Testimonials
Our 5 star service
Liam Naylor
Holly at flex is absolutely fantastic, I had to start sessions due to an RTC and I have been made to feel welcome as soon as I came through the doors. Highly recommend 10/10
Brad Graham
I've used Flex Health for multiple injuries over the years, and I honestly can't recommend them enough. I've seen several of their physios, but mainly Alex Chester, who has been absolutely fantastic every time.
Sylvia Usher
Lisa at Flex Health helped me to almost enjoy exercises, and I do look forward to coming! Coming to Flex Heath, with the advantage of the gym facilities, rebuilt my confidence in walking outside my garden.
Frequently Asked Questions
Q: Is cerebral palsy progressive?
A: The original brain injury does not worsen, but secondary complications (muscle contractures, joint degeneration, pain) can develop if not addressed early.
Q: Can CP be cured?
A: There is currently no cure. Treatment focuses on maximizing functional abilities, reducing discomfort, and preventing secondary problems.
Q: At what age should therapy start?
A: As soon as a diagnosis is confirmed—often within the first year of life—early intervention yields the greatest long‑term benefit.
Q: Will my child outgrow spasticity?
A: Spasticity may change with growth, but it typically persists into adulthood. Ongoing therapy and periodic reassessment help adapt treatment.
Q: Are there any lifestyle restrictions?
A: Most activities are possible with adaptations. Encourage participation in school, sports, and community events; tailor equipment as needed.
Q: How do I choose the right assistive device?
A: Work with a certified orthotist or physiotherapist who evaluates mobility goals, body mechanics, and home environment before recommending a device.


